Since 1991, conflict and statelessness profoundly affected the health care system in Somalia. After the collapse of the central government and the descent into civil war, many efforts to restore a central government were unsuccessful. Powerful internal forces and regional dynamics resulted in a state of chaos. The impact of lack of governance has resulted in a generation without adequate access to social services and the collapse of public institutions for health and welfare. Despite the success of some business sectors, Somalia is marred with widespread social and economic problems and a dire lack of public social amenities. In 1991, the North West region declared an independent republic of Somaliland. Later, in 1998, the northeast declared itself as autonomous state of Puntland. The south central zones of Somalia remain locked in intermittent conflict and violence.
Literature review indicates, even before the outbreak of the internal conflict, the health systems in Somalia were rather weak and underfunded. After 19 years of conflict, the health systems in Somalia remains underdeveloped poorly resourced, inequitable and unbalanced. It struggles to provide services to a limited number of Somalis against crushing constraints.
Insecurity, geographical challenges and nomadic populations, unstructured and unskilled workforce, lack of motivation and division, uncertainty about the political future and administrative setting are key issues that the Somali Health system is facing. The ministry of health’s ability to coordinate and monitor health services is almost absent.The public health care network is small. It most relies on national and international NGO’s that are concentrated in towns and secure areas. The health workforces are few, under skilled and ageing often-engaged in private and public practices.
Limited access due to insecurity in Central and south Somalia and South Sudan has restricted health activities, contributing to the spread of diseases such as acute respiratory tract infections, obstetrical problems, anaemia, and sexually transmitted infections. In addition, injuries resulting from armed conflict are common but few health facilities have the capacity to treat them. In some areas, war-damaged hospitals and clinics have been rebuilt and qualified health professionals are returning to practices, but the overall health situation in Somalia remains worse with some of the worst health indicators in the world.
SFH Integrated health program envision to:
- Increased access to essential package of health services, maternal health services and improved quality of care for the target populations.
In Somalia-Lower Juba, SFH:-
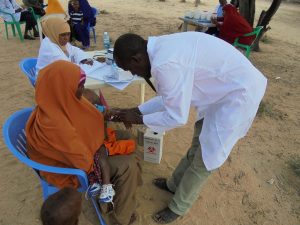
- Support 1 Hospital, 4 MCH and 6 health posts with staff, drugs and medical equipment’s to provide diagnosis, treatments and emergency referrals.
- Provides refresher trainings to all levels of health workers in our static health facilities and health post, to ensure timely and quality responses are delivered in case of outbreaks and in post recovery situations.
- Health centres provides skilled birth attendance and emergency obstetric care services.
- All health facilities provides free PNC /ANC services
In general, our health facilities record an average annual consultation, treatments and referrals of 12,000 patients.
NUTRITION
The precarious nature of worsening nutrition situation in the region, particularly South-central Somalia is demonstrated in all nutrition assessment conducted over the last 6 years. The nutrition indicators in Somalia and South Sudan depicts the worst in the globe with 1 in every 6 child acutely malnourished and GAM rates exceed the 15percent WHO emergency threshold for almost ¾ of a decade now.
In line with those preliminary background and the nutrition cluster response plans, SFH’s nutrition programs endeavoured:
- Increased access to nutrition interventions aimed at preventing, identifying and treating moderate and severe malnutrition among children under the age of 5years, pregnant and lactating women.
In all the 22 nutrition centres (Fixed and Outreach)we are currently running our program focus:
- Children with SAM are able to access out-patient therapeutic feeding at our well-equipped centres with fully trained staff.
- Children and PLW with MAM are able to access targeted supplementary feeding program (TSFP) and appropriate IYCF sessions.
- Community health workers and Volunteers are trained in screening for acute malnutrition, active case finding and follow up of program beneficiaries.
BNSP component is integrated with the administration of all nutrition services. BNSP (Management of acute malnutrition, micronutrient supplementation, immunizations, Deworming, Promotion and support for optimal IYCF, promotion and support for optimal maternal nutrition and care, prevention and management of common illnesses (anemia, diarrhea, pneumonia, kalazar, where appropriate).
Since the inception of our Somalia programs, we have successfully identified and provide appropriate treatments to 74,870 <5 children and Pregnant & Lactating women. Beside these 7150 complicated cases were referred for specialized care.